Hysteroscopy is a procedure inspection condition of the neck and inside of the uterus. This procedure can be used fordiagnosing disease or causes of infertility and help treat abnormalities in the uterus.
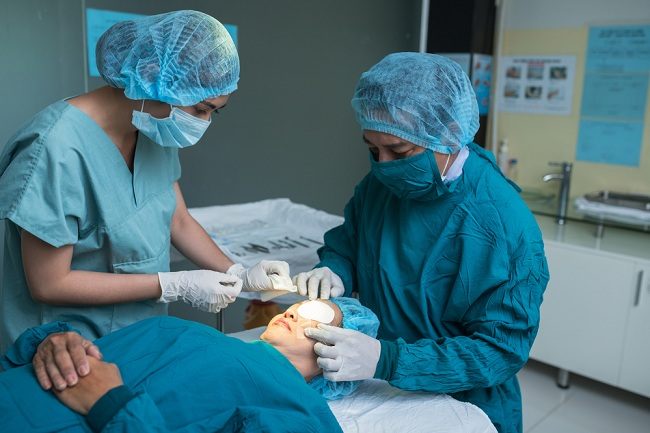
Hysteroscopy is performed using a hysteroscope, which is a thin, flexible tube with a camera on the end. The device is inserted into the uterus through the vagina, so the doctor can check the condition of the inside of the uterus through a monitor screen.

There are two types of hysteroscopy methods, namely diagnostic hysteroscopy and operative hysteroscopy. Diagnostic hysteroscopy is used to see the condition of the uterus. However, if an abnormality is found on examination that can be corrected immediately, this procedure becomes an operative hysteroscopy.
Hysteroscopy Indications
Doctors may perform a hysteroscopy with the aim of:
- Find out the cause of abnormal bleeding from the vagina, such as continuous menstruation or bleeding after menopause
- Investigating the causes of repeated miscarriages (at least 2 times in a row) or the causes of women having difficulty conceiving after 1 year of undergoing a pregnancy program
- Detect abnormal uterine tissue, such as scar tissue, fibroids, and uterine polyps
- Detect uterine or fallopian tube deformities
- Take a sample of suspected abnormal tissue (biopsy) for analysis in the laboratory
- Removing abnormal tissue in a small uterus
- Correcting abnormalities at the end of the fallopian tube
- Removing contraceptives intrauterine device (IUD) that is difficult to remove manually
- Assist in sterilization procedures, namely permanent contraception in women by closing the fallopian tubes
Hysteroscopy Warning
Patients with the following conditions are not allowed to undergo hysteroscopy:
- Are pregnant, because it can trigger a miscarriage
- Suffering from cervicitis
- Suffering from cervical cancer
- Have a wide uterine cavity or the length of the uterus is more than 10 cm
- Experiencing very severe bleeding in the uterus
- Suffering from pelvic inflammatory
Before Hysteroscopy
Before undergoing a hysteroscopy, there are several things that patients need to pay attention to, namely:
- Ask your doctor if you need to fast before the procedure.
- Avoid using douche (vaginal cleansing soap), tampons, or medications that are inserted into the vagina.
- Inform your doctor if you are menstruating or if the hysteroscopy schedule coincides with your expected period.
- Tell your doctor about any medicines, supplements, or herbal products you are currently taking.
- Invite relatives or family to drop off, pick up, and accompany you during and after the procedure.
- Take a pain reliever, such as ibuprofen or paracetamol, 1 hour before the procedure, if you are concerned that the procedure will cause discomfort. However, consult your doctor first.
Hysteroscopy Procedure
Before the procedure begins, the patient will be asked to remove all lower clothing. Next, the doctor will perform a hysteroscopy with the following steps:
- The patient will be asked to lie on his back with his knees bent and wide apart.
- The doctor may administer local anesthesia (the patient remains awake) or general anesthesia (the patient is asleep), depending on the patient's condition and how complicated the procedure is.
- The doctor will clean the patient's vagina with an antiseptic solution.
- The doctor will insert a speculum into the vagina to support the vaginal wall so that it can continue to open.
- The doctor will slowly insert the hysteroscope through the vagina, then into the cervix, and finally into the uterine cavity. At this stage, the patient may experience discomfort or cramping as if he was menstruating.
- The doctor will insert sterile gas or liquid into the uterus, so that the uterus expands and the image of the uterine cavity captured by the camera can be more clear.
- The doctor will see and analyze the condition of the inside of the uterus through a monitor screen that is connected to the camera on the hysteroscope.
- If tissue is found that needs to be removed, either for surgery or a biopsy, the doctor will insert a special instrument through the hysteroscope to remove the tissue.
Hysteroscopy can last for 15–60 minutes. The length of this procedure depends on what type of action is being performed.
After Hysteroscopy
After the procedure is complete, the patient can go home immediately. However, the patient is advised to rest first in the treatment room for a few hours, until the effect of the anesthetic wears off.
For a few days after the procedure, the patient may experience mild cramping and bleeding. The doctor will give you painkillers to relieve the cramps you feel.
The results of operative hysteroscopy and some diagnostic hysteroscopy can be communicated to the patient immediately after the procedure is completed. However, for diagnostic hysteroscopy that requires a biopsy, the results are usually not available for 2-3 weeks after the procedure.
The following are some of the abnormalities that can be found on diagnostic hysteroscopy:
- Myomas, uterine polyps, or other abnormal growths, including endometrial cancer
- Scar tissue in the uterus, as in Asherman's syndrome
- Abnormal size or shape of the uterus
- Blockage in the fallopian tube
The doctor will discuss the results of the hysteroscopy with the patient, especially if further treatment is needed to overcome the problems found. However, if no abnormalities are found on hysteroscopic examination, further examination may be needed to determine the cause of the patient's complaints.
Complications Hysteroscopy
Hysteroscopy is a safe procedure. However, in rare cases, this procedure causes complications such as:
- Bleeding
- Uterus infection
- Damage to the uterus from a puncture or tear
- Damage to organs around the uterus, such as the bladder
- Allergic reaction to the fluids used during the procedure