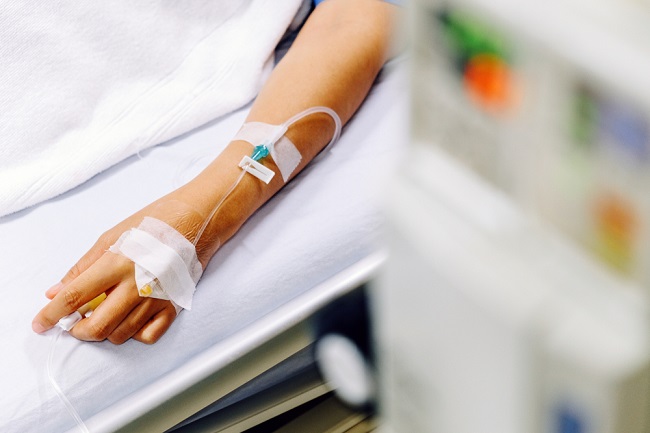
Alcohol-related liver disease is liver damage due to excessive and long-term alcohol consumption. Such alcohol consumption can cause the liver to experience inflammation, swelling, and scarring or cirrhosis which is the final stage of liver disease. Alcohol-related liver disease is often only detected after the liver has suffered further damage.

The liver is one of the organs of the body with many functions, namely to filter toxins from the blood, regulate blood sugar and cholesterol levels, help the body eradicate infections and diseases, and help the process of digestion of food. The liver is very flexible and capable of self-renewal. New cells will grow when old cells die. However, this abuse of alcohol consumption can reduce the ability of liver cells to renew themselves. As a result, sufferers will experience serious liver problems and permanent liver damage.
A person is said to have consumed alcohol excessively if he drank more than 14 units of alcohol within 1 week. One unit of alcohol = 25 ml.
Types of Alcohol-related Liver Disease
There are three types of alcohol-related liver disease, namely fatty liver, alcoholic hepatitis, and alcoholic cirrhosis. Fatty liver or fatty liver is an early stage liver disorder that can cause the liver to swell. This disease can be overcome by stopping alcohol consumption, for at least 2 weeks or until the liver condition becomes normal.
Next is alcoholic hepatitis which is characterized by inflammation of the liver. It is at this stage that a person becomes aware of alcohol-related liver damage. Alcoholic hepatitis can be recovered if the liver disorder that occurs is still relatively mild, and the patient stops drinking alcohol forever. However, if it is classified as serious, this condition can endanger the life of the sufferer.
The third type of alcohol-related liver disease is alcoholic cirrhosis. This condition is the most severe type of liver disease. In this condition, normal liver tissue becomes damaged and scar tissue develops, so the liver does not function. Although this condition is irreversible, quitting the habit of drinking alcohol can prevent further liver damage and thus increase life expectancy.
Symptoms of Alcohol-related Liver Disease
Symptoms of alcohol-related liver disease sometimes go unnoticed until the liver has been severely damaged. However, the initial symptoms that are generally felt by sufferers are loss of appetite, fatigue, feeling unwell, abdominal pain, and diarrhea.
Meanwhile, based on the type of alcohol-related liver disease, the specific symptoms that can appear are:
- Fatty liver - Pain in the upper right abdomen.
- alcoholic hepatitis - fever, weakness, nausea, yellow skin, right abdominal pain, elevated white blood cell levels, and swollen and tender liver.
- alcoholic cirrhosis - Swollen spleen, ascites (buildup of fluid in the abdominal cavity), and portal hypertension (increased pressure on blood flow to the liver).
At an advanced stage where liver damage is getting worse, serious symptoms can be more visible, namely:
- The stomach is getting bigger because of ascites
- Fever
- Itchy skin
- Hair loss
- Significant weight loss
- Weak body and muscles
- Insomnia (difficulty sleeping)
- Loss of consciousness
- Tends to bleed or bruise easily
- Vomiting blood that is black in color due to rupture of esophageal varices.
Causes of Alcohol-related Liver Disease
Alcohol-related liver causes are excessive alcohol consumption. Based on the time period, the disease that arises can be different, namely:
- Alcohol consumption in excess of the recommended limit in a short period of time - this behavior can lead to fatty liver and alcoholic hepatitis.
- Excessive alcohol consumption over the years - this habit can lead to alcoholic hepatitis and cirrhosis.
A person's risk for alcohol-related liver disease will be greater if:
- Have a family member with a history of this disease
- Having poor nutrition
- Obesity
- Have you ever had a heart problem before?
Alcohol-related Liver Disease Diagnosis
The diagnosis of alcohol-related liver disease begins with an examination of the patient's symptoms and alcohol consumption habits, followed by a physical examination. To determine alcohol-related liver disease, several investigations are needed, including:
- Blood test. This examination is done by examining the blood to identify liver disorders that occur in the patient. If abnormal blood clotting levels are found, it can indicate significant liver damage. On liver function tests, especially gamma-glutamyltransferase (GGT), aspartate aminotransferase (AST) or SGOT, as well as alanine aminotransferase (ALT) or SGPT, the doctor can determine the type of liver disorder. The SGOT level, which is twice as high as the SGPT level, indicates the patient has alcohol-related liver disease.
- Scanning. The type of scan that can be done is ultrasound, which uses sound wave technology to display detailed images of the liver. However, ultrasound cannot detect subtle changes in the liver, so a CT scan is required. This test can help diagnose cirrhosis, portal hypertension, and liver tumors. Another scan that can be done is an MRI. Examination with a tool that uses a strong magnetic field and sound waves can display a more detailed picture of the heart.
- Endoscopy. This examination uses an endoscope, which is a flexible tube equipped with a light and video camera at the end. This tool is inserted through the throat until it reaches the stomach. If the endoscope detects swelling of the veins (varicose veins), it can be a sign of cirrhosis.
- Liver biopsy. This examination is done by taking a sample of liver cells to be brought to the laboratory and examined under a microscope. Liver biopsy aims to assess the severity of the scar tissue and the cause of the damage.
Alcohol-related Liver Disease Treatment
Until now, there is no specific drug that can treat alcohol-related liver disease. The main treatment that can be done is to help the patient stop drinking alcohol to prevent further liver damage.
For patients with alcohol-related liver disease, it is highly recommended to be able to stop consuming alcohol for life. If you can't get rid of addiction, then the patient must be willing to follow a rehabilitation program for alcohol addiction.
In addition to advice to stop the habit of consuming alcohol, doctors can also provide vitamin supplements. Many people with alcohol-related liver disease have vitamin B complex and vitamin A deficiencies, which can lead to anemia or malnutrition. Therefore, in order to prevent these complications, patients are recommended to take vitamin B complex and vitamin A supplements. However, it should be remembered that vitamin A supplements can only be given to patients who have stopped consuming alcohol, because taking vitamin A supplements and alcohol at the same time can be dangerous. .
In addition, a balanced diet can also help sufferers get adequate nutrition. Patients are advised to avoid salty foods to prevent the risk of fluid buildup in the legs and stomach. Liver damage can also make the body unable to store glycogen or carbohydrates. If there is a lack of carbohydrates, the body uses muscle tissue as energy so that it can make the body and muscles weak. Therefore, patients are advised to eat healthy snacks between meals to increase calorie and protein levels.
Operation
Treatment with liver transplant surgery may be recommended by a doctor if the liver can no longer function properly, or there is cirrhosis that leads to liver failure. Patients may consider receiving this procedure if they have liver failure that continues to worsen despite stopping alcohol consumption, are committed to abstaining from alcohol for the rest of their lives, and are in good health and able to undergo this operation.
Alcohol-related Liver Disease Complications
Several complications can occur after the patient suffers from alcohol-related liver disease. A complication that occurs from hepatitis and alcoholic cirrhosis is portal hypertension, in which blood pressure in the veins around the liver increases. When scar tissue begins to grow on the liver, it is difficult for blood to move through the tissue, so the pressure in the blood vessels leading to the liver increases. At that time, the blood is looking for an alternative way to return to the heart, namely the small blood vessels around the esophagus or esophagus. The amount of blood that flows, makes these small blood vessels dilate and are known as esophageal varices. If the pressure continues to increase, the walls of the varicose veins can rupture and cause bleeding. This bleeding can cause complaints of vomiting blood and bloody stools, with a black color.
Hypertension in the blood vessels around the liver, known as portal hypertension, can also lead to a buildup of fluid in the stomach and around the intestines, known as ascites. If in the early stages, ascites can be treated with diuretic tablets. However, when the accumulation of fluid increases, the fluid must be removed by placing a long tube under the skin to drain the fluid (ascitic puncture or paracentesis). The emergence of ascites in patients with cirrhosis is at risk of causing peritonitis or infection in the abdominal cavity which is dangerous.
In people with alcohol-related liver disease, especially hepatitis or alcoholic cirrhosis, the liver cannot function to remove toxins from the blood. As a result, the level of toxic ammonia in the blood is higher. This condition is known as hepatic encephalopathy. This complication requires hospitalization to support body functions and administration of toxin-eliminating drugs from the blood.
Patients with alcohol-related liver disease are also prone to developing liver cancer. It is estimated that 3-5% of people with alcoholic cirrhosis can develop liver cancer.